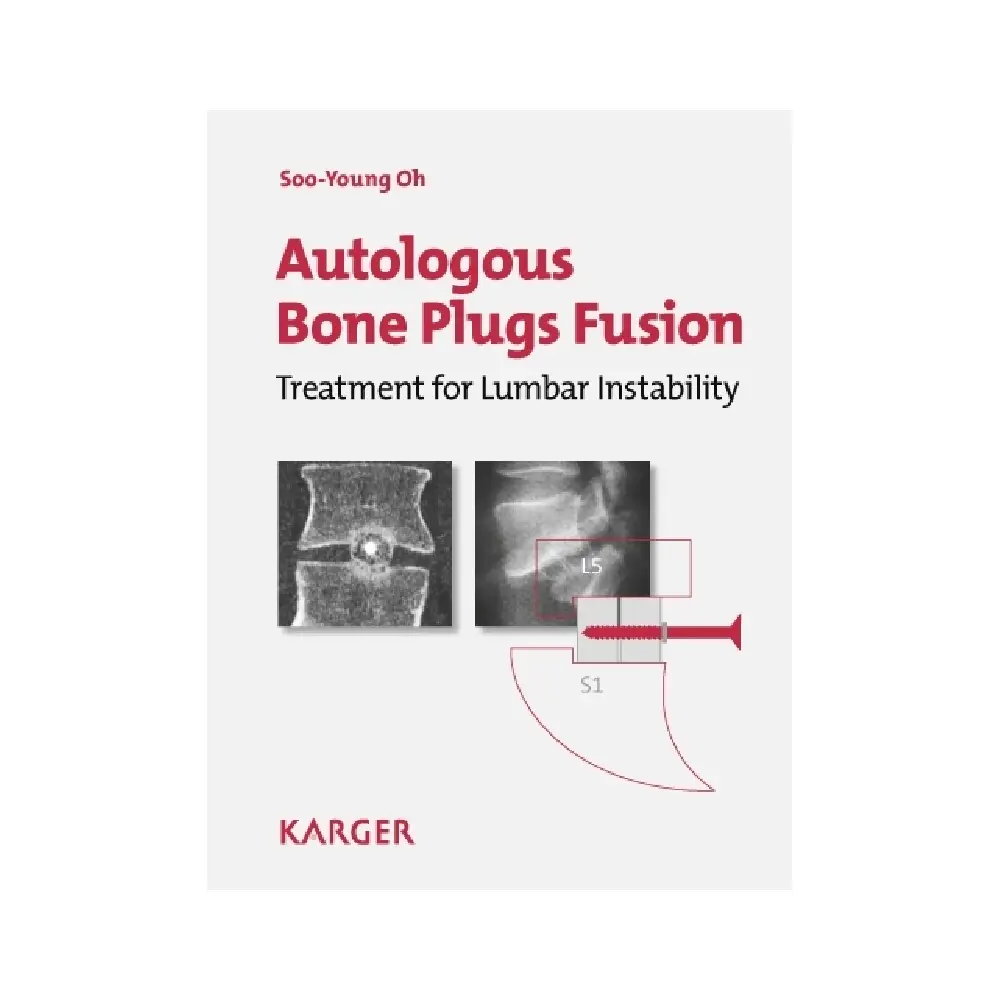
Autologous Bone Plug Fusion: A Treatment for Lumbar Instability
Lumbar instability refers to abnormal motion between vertebrae in the lower spine, often causing mechanical back pain, radiculopathy, and functional impairment. Surgical stabilization is indicated when conservative measures fail. Among fusion techniques, autologous bone plug fusion is widely used because it utilizes the patient’s own bone to create a biological bridge that ultimately solidifies vertebral segments while preserving spinal mechanics and minimizing rejection.
This approach centers on three core concepts:
-
Biological osteogenesis using autologous bone.
-
Controlled immobilization of the affected segments.
-
Mechanical stability provided by internal fixation — in many cases using specialized instrumentation such as the Oh’s Screw.
Below is a breakdown of the surgical strategy.
1. 3E Criteria
The 3E criteria are used to determine candidacy for lumbar fusion:
E1 — Evidence of Instability
Instability must be proven using objective diagnostic criteria:
-
Dynamic radiographs (flexion/extension X-rays) showing >3–5 mm translation or >10–15° angular motion between adjacent vertebrae.
-
MRI evidence of disk degeneration, facet joint effusion, or ligamentous laxity.
-
Positive clinical correlation — mechanical back pain exacerbated by movement and relieved by stabilization.
E2 — Exhaustion of Conservative Therapy
Patients should have undergone appropriate non-surgical treatment:
-
Physical therapy with core strengthening and stabilization exercises.
-
Injections (epidural steroids, facet blocks) to confirm pain generators.
-
Activity modification and analgesic regimens.
Failure of these therapies over a reasonable timeframe (typically 3–6 months) warrants considering fusion.
E3 — Expected Functional Gain
Surgery should be justified by:
-
Likelihood of meaningful pain relief
-
Improved activity and quality of life
-
Prevention of progressive neurologic deficit
-
Relative surgical risk acceptable for the patient’s health
Only patients meeting all three criteria (E1 + E2 + E3) are deemed appropriate candidates for surgical fusion.
2. Technical Operative Notes
Preoperative Planning
-
Imaging: High-resolution MRI and CT scans to localize pathology, assess bone quality, and plan graft harvest.
-
Bone Graft Assessment: Harvest sites should be evaluated — typically the iliac crest — for sufficient autograft volume.
-
Neuromonitoring planning: Somatosensory and motor-evoked potentials may be used intraoperatively.
Surgical Steps
a) Approach
Most commonly performed through a posterior open approach:
-
Patient is placed prone on a radiolucent operating table.
-
Midline incision and subperiosteal dissection expose the target segments.
-
Facet joints and lamina may be partially removed (laminotomy/facetectomy) to decompress nerve roots.
b) Preparation of Fusion Beds
-
Decortication: The posterior elements (transverse processes, lamina) are decorticated using high-speed burrs to expose vascular cancellous bone — essential for graft incorporation.
-
Interbody Space: If an interbody fusion is planned (PLIF or TLIF), the disk space is debrided and prepared to receive graft material.
c) Harvesting Autologous Bone Plugs
-
A separate incision is made over the iliac crest.
-
Cancellous bone is harvested in plug/strip form using curettes or trephines.
-
Meticulous hemostasis in the donor site is crucial to minimize pain and complications.
-
Bone plugs are sized to fill decorticated fusion beds or interbody cages.
d) Graft Placement
-
Bone plugs are inserted into the prepared fusion sites.
-
If an interbody cage is used, cancellous plugs are packed within the cage to maximize osteogenic potential.
-
Care is taken to ensure tight fit and good contact with host bone.
e) Instrumentation
Internal fixation is essential for immediate stability. Options include:
-
Pedicle screws and rods
-
Hooks and wires
-
Oh’s Screws (see next section)
Instrumentation maintains immobilization to allow biological fusion.
f) Closure
-
Layered closure of muscle, fascia, and skin.
-
Drains may be placed to prevent hematoma.
3. The Functioning of the Oh’s Screw
The Oh’s Screw is a specialized pedicle fixation device used in lumbar fusion. Its design is optimized for stability in compromised bone and ease of insertion.
a) Design Features
-
Cannulated shaft: Allows guidewire-assisted placement.
-
Thread geometry: Aggressive threads enhance purchase in cancellous bone, improving pullout strength.
-
Expandable tip (optional): Some designs allow distal expansion once inserted, increasing surface area contact.
b) Biomechanical Role
The Oh’s Screw serves multiple functions:
Fixation
-
It anchors the vertebrae via pedicles — the strongest portion of lumbar vertebrae.
-
Once connected with rods, it resists:
-
Axial loads
-
Shear forces
-
Torsion
-
This stabilization is crucial while biological fusion develops.
Load Sharing
-
The threaded design distributes mechanical stress across vertebral bodies and graft sites.
-
This minimizes stress concentration and risk of hardware failure.
Facilitation of Fusion
-
Stable fixation prevents micro-motion at the graft site—crucial because excessive motion suppresses osteogenesis.
-
The Oh’s Screw provides rigid immobilization, creating a favorable biological environment for bone healing.
Conclusion
Autologous bone plug fusion remains a gold-standard surgical option for lumbar instability when conservative measures fail and when patients meet stringent 3E criteria. Using the patient’s own bone enhances biological integration, while meticulous surgical technique promotes optimal fusion. Oh’s Screws and similar fixation devices provide necessary mechanical stability, ensuring a high likelihood of successful arthrodesis and clinical improvement.











Reviews
There are no reviews yet